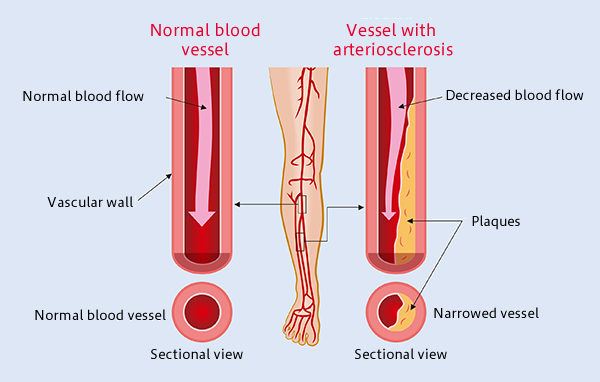
Atherosclerosis obliterans grade IV: Application of Autologous Stem Cells
Atherosclerosis is the most common form of arterial occlusive disease in adults. About 15 percent of adults over 55 years of age suffer from critical ischemia, the most severe form of this disease.
Due to the gradual aging of the population and the growing number of people in their third age group, a number of studies have been conducted in order to improve the prognosis of atherosclerosis obliterans and to find alternatives to the mutilation of the extremities. As a general rule, chronic ischemia of the lower limbs should be treated to alleviate symptoms, particularly pain, prevent disease progression, and reduce the rate of amputations. In most patients with critical ischemia, the main goal is to preserve the affected limb.
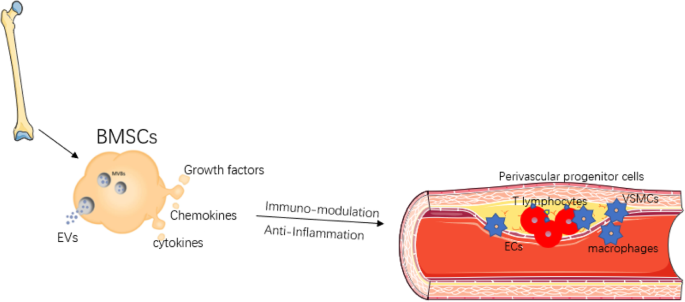
The development of regenerative medicine is closely linked to the development of new knowledge about embryonic and adult stem cells, as well as the regenerative and therapeutic potential of stem cell therapy. The use of adult stem cells in the treatment of peripheral artery diseases has been demonstrated as a therapeutic agent for inducing angiogenesis. Recent preclinical studies as well as the pioneering clinical studies indicate that bone marrow-derived mononuclear cells (MBMCs) can enhance tissue vascularization in ischemic limbs, with results similar to those obtained with peripheral blood stem cells supply.
Cuba presented the first studies carried out in 2004 at the Institute of Hematology of the “Enrique Cabrera” hospital in Havana City, which achieved encouraging clinical results and had very few adverse effects in recent years.
A progressive rise in the accumulated experience with stem cells was also observed in Pinar del Rio in 2005, as the first 10 cases were carried out. The rising ease of obtaining this type of cell has made research and applications with these cells advance rapidly with great expectations in terms of clinical application.
A study published by Dia-Diaz, et al. in the Journal of Medical Sciences of Pinar del Rio examined 296 patients with grade IV atherosclerosis obliterans between 2009 and 2019. During the study, autologous stem cells were injected intramuscularly from peripheral blood. Within four weeks, pain relief was observed, as well as an increase in the pain-free claudication distance. Angiography after treatment revealed collateral vessel formation. The limb was saved in 201 patients (68%), while 95 cases (32%) presented amputation criteria. Complications were not reported following the procedure.
The study demonstrated the effectiveness of the implantation of autologous stem cells obtained from peripheral blood, as well as the favorable evolution of patients, clinical improvement of rest pain, walking distance without claudication and ankle-brachial pressure index.
We still need to explore a lot of ground, in terms of these and other conditions. You can learn more about regenerative medicine and stem cells by enrolling in our international certification program at www.issca.us
- Published in Corporate News / Blog
How much does exosome therapy cost?
Exosome therapy is the new buzz in the regenerative medicine industry because of how it can repair and regenerate your cells and tissues.
Exosome therapy is safer compared to other cellular therapy because it’s a cell-free therapy with no risk of rejection.
Exosome therapy will be beneficial to you if you’re dealing with conditions such as sport injuries, tissue regeneration, hair loss, erectile dysfunction, chronic pain and so many other applications .
In this article, you’ll be learning the cost of exosome therapy and how you can benefit from exosome therapy.
How the cost of exosome therapy is determined
All cells produce exosomes, which are microvesicles that contain biochemical and genetic information.
Hence, the cost of an exosome product (used in exosome therapy) will depend on what type of cell line (raw tissue source) used to extract the exosomes.
The first factor to determine the cost of an exosome product depends on the quality of the tissue source.
The most commonly used tissue types are cord blood, amniotic fluid and mesenchymal cell cultures.
Exosomes derived from mesenchymal cell cultures are the most difficult to obtain but offer the greatest therapeutic potential.
How much does exosome therapy cost?
The average cost of exosome therapy is $4,900, but the price can be anything from $3,500 – $6,500.
It’s also important to note that the price depends on your specific needs and your treatment plan, as decided by the doctor.
The doctor will schedule a consultation with you to determine your personalized treatment plan.
The exosome therapy can either be given as an IV infusion or as localized injections, depending on the purpose of the therapy.
Exosomes are very useful to revitalize, rejuvenate, restore, and reduce inflammations in the body.
Here are some ways you can benefit from exosome therapy
Hair loss therapy
If you’re in the early stages of hair loss, with exosome therapy you can regenerate your hair whether you’re a man or woman. After exosome therapy, you’ll start seeing new hair growth in as little as two to three months with very significant results showing 6 months or 1 year later.
Chronic pain
In case you’re experiencing chronic pain due to degenerative conditions such as arthritis, exosomes can help to subdue the pain by regenerating the cells and helping the body work better.
Degenerative conditions
If you’re struggling with degenerative medical conditions such as osteoarthritis and musculoskeletal injuries, exosome therapy can help your body repair the damage done to your cells by these conditions, prevent them from getting better, and help you to feel better.
Skin therapy
Exosome therapy can reduce inflammation in the skin by improving the strength and elasticity of the skin.
Anti-aging
If you would like to retain your youthful glow, exosome therapy can make you feel young again by rejuvenating your skin due to its ability to reverse the cells dying due to aging.
Where can you get exosome therapy?
Cellular hope institutes provide exosome therapy for patients looking for better outcomes for various conditions.
The exosomes used at Cellular Hope Institute are obtained from umbilical cord tissue that is discarded after a new birth , which means these Exosomes have not been exposed to any contaminating or toxic agent because our cells are as healthy as our body. This gives it a higher capacity to regenerate your cells and tissues.
- Published in Corporate News / Blog
Culture Expanded MSCs
Mesenchymal Stem Cells (MSCs) are the most commonly used cells in stem cell therapy and regenerative medicine, due to their high and multi-potency. Mesenchymal Stem Cells (MSCs) can be isolated from different tissues in the body.
In this article, you’ll be learning about culture-expanded MSCs, how MSCs can be expanded, The potency of MSCs and the type of cells they can differentiate into.
What are culture expanded Mesenchymal Stem cells?
Mesenchymal stem cells are high potent cells used for cellular therapy and isolated from different parts of the body. Mesenchymal stem cells can be used to improve the patient outcome in diseases and conditions such as autoimmune diseases, degenerative diseases, nerve damage, diabetes mellitus, bone problems etc.
For every patient, millions of mesenchymal stem cells are needed and the exact amount varies according to disease, route of administration, administration frequency, weight, and age of patient.
Mesenchymal stem cells are expanded in a culture media, on a large scale in order to obtain the required quantity of cells needed for cellular therapy.

Culture expanded MSCs: How does it work?
Expanding Mesenchymal stem cells in a media involves step by step process of isolation and expansion.
Mesenchymal Stem Cells Isolation
Mesenchymal stem cells can be isolated from different tissues in the human body such as adipose tissues, dental pulp, human bone marrow, umbilical cord tissue, umbilical cord blood, peripheral blood and synovium.
Mesenchymal stem cells are expanded in culture to increase their yield and amplify their desired functions and potency.
Although the population of Mesenchymal Stem Cells obtained will vary from donor to donor, here are some steps to follow:
- Acquire fresh tissue extracts in strictly aseptic conditions, to maintain purity.
- To remove any cell clusters, you have to filter the cell suspension with a 70-mm filter mesh
- Use a centrifuge to roll the cells for about 5 minutes at 500g
- Suspend the cells again the cells to measure the cell viability and yield using Trypan blue exclusion
- Use in T75 culture dishes to culture the cells in 10 mL of complete MSC medium at a density of 25 × 106 cells/mL. You can then go on to Incubate the plates at 37 °C with 5% CO2 in a humidified chamber without any interruption.
- When it’s past 3 h, remove the non-adherent cells that accumulate on the surface of the dish by changing the medium and replacing it with 10 mL fresh complete medium.
- After an additional 8 h of culture, add 10ml fresh complete medium as a replacement for the existing medium. You’ll have to repeat this step every 8 h for up to 72 h of initial culture.
- Cells can be frozen in MSC growth media plus 10% DMSO (D2650) at a density of 2X106 cells/vial.
Expansion of Mesenchymal Stem Cells in a culture media
Culture expanded mesenchymal cells undergo various stages from the preparation of the culture plate, thawing of Mesenchymal stem cells, and the actual expansion of Mesenchymal stem cells.
The reason behind the cultural expansion of Mesenchymal stem cells is to get them to differentiate into other cell types such as osteoblast, adipocyte, and mesenchymal stromal cells.
In preparation, to expand MSCs in a culture media, you need a culture ware. You can get one plastic or glassware plate and coat it with a sufficient amount of 0.1% gelatin. Don’t forget to aspirate the gelatin solution from the coated plate or flask before you use it.
The next step involves the thawing of the Mesenchymal stem cells, and here are a few steps for you to follow:
After the recommended culture medium and coated culture ware is ready and on standby, remove the vial of Mesenchymal Stem Cells from liquid nitrogen and incubate in a 37C water bath and pay close attention to it, until all the cells are completely thawed. The extent of completely thawed frozen cells and how fast, are what determines the cell viability.
Once the cells have thawed completely, take steps to avoid contamination by disinfecting the walls with 70% ethanol, before you proceed to the next step.
Place the cells in a hood, and carefully transfer the cells to a sterile tube with a pipette (1 or 2ml pipette), Do this in such a way to prevent bubbles.
Then, add drops of Mesenchymal Stem cell expansion medium that have been pre-warmed to 37C to the tube containing the Mesenchymal stem cells.
Be careful to take your time when adding the medium to avoid osmotic shock which could lead to decreased viability.
Proceed to mix the suspension slowly by pipetting up and down two times while avoiding any bubbles.
Place the tube in a centrifuge and centrifuge the tube at 300 x g for 2-3 minutes to roll the cells, and you should not vortex the cells.
After this, then decant as much of the supernatant as possible. These steps are necessary to remove residual cryopreservative (DMSO).
Suspend the cells in a total volume of 10 mL of Mesenchymal Stem Cell Expansion Medium again or any alternative of choice, pre-warmed to 37 °C, containing freshly added 8 ng/mL FGF-2 (F0291).
The next step involves placing the cell suspension onto a 10-cm tissue culture plate or a T75 tissue culture flask.
Maintain the cells in a humidified incubator at 37 °C with 5% CO2.
The next day, exchange the medium with fresh Mesenchymal Stem Cell Expansion Medium (pre-warmed to 37 °C) containing 8 ng/mL FGF-2*. Replace with fresh medium containing FGF-2 every two to three days thereafter.
Isolate the cells when they are approximately 80% confluent, using Trypsin-EDTA and passaged further or frozen for later use.
Expansion of Mesenchymal Stem Cells
Once the cells are actively proliferating and have reached a confluence of approximately 80% (before 100%), you should subculture the cells.
Then remove the medium from the 10-cm tissue culture plate containing the confluent layer of human mesenchymal stem cells, carefully and apply 3-5 mL of Trypsin-EDTA Solution, before proceeding to incubate in a 37 °C incubator for 3-5 minutes.
Crosscheck the culture to see if all the cells are completely detached. Then, add 5 mL Mesenchymal Stem Cell Expansion Medium to the plate.
Swirl the plate mildly to mix the cell suspension. Transfer the separated/isolated cells to a 15 mL conical tube.
Centrifuge the tube at 300 x g for 3-5 minutes to pellet the cells.
Throw the supernatant away and apply 2 mL Mesenchymal Stem Cell Expansion Medium (pre-warmed to 37 °C) containing 8 ng/mL FGF-2 to the conical tube and completely suspend the cells again. Remember not to vortex the cells.
Then, use a hemocytometer to count the number of cells.
Plate the cells at a density of 5,000-6,000 cells per cm2 into the appropriate flasks, plates, or wells in a Mesenchymal Stem Cell Expansion Medium containing 8 ng/mL FGF-2.
Cells can be frozen in MSC growth media plus 10% DMSO (D2650) at a density of 2X106 cells/vial.
Functions of Culture Expanded MSCs
Mesenchymal stem cells are required to be expanded in order for them to be used clinically for therapeutic purposes.
The culture expanded MSCs can be induced to differentiate into adipocytes, osteocytes, hepatocytes, chondrocytes, tenocytes and cardiomyocytes.
Because of its potential to differentiate into different kinds of cells in the body, it can be used to manage liver problems, heart problems, joint and bone problems etc.
Mesenchymal stem cells are also used in tissue regeneration and modulation of the immune system. They possess anti apoptotic, angiogenic, anti fibrotic, and anti-oxidative properties.
However, the quantity of MSCs isolated from body tissues is not enough for clinical and therapeutic applications.
This is why MSCs are expanded in culture to increase their yield for desired therapeutic effect.
- Published in Corporate News / Blog
Why cellular therapies have become a standard in clinics that are betting on biological medicine
Cellular therapy is fast becoming a standard therapy in many regenerative clinics today. Many doctors are no longer questioning the safety and effectiveness of stem cell therapy. This is because various stem cell studies are already describing the benefits of stem cells for patients who are living with chronic and autoimmune health conditions.
This article will be talking about why stem cell therapy have become a standard therapy in clinics, the paracrine effect of stem cells, and other reasons why doctors are adopting stem cells in their clinics.
Benefits of stem cell therapy
Stem cell therapy is an important innovation in medicine because of its regenerative power in the human body. Most disease states are characterized by damaged cells, tissues and organs, which is where stem cell therapy comes in. In stem cell therapy, stem cells are administered into the human body and it replaces the cells damaged by disease or health disorders.
Stem cell research has revealed two major ways of using stem cells to rebuild defective and damaged cells. One of these ways can be seen in procedures like bone marrow transplant, where stem cells are used to replace the damaged cells by engraving, and they then differentiate into the proper cell type. Another mechanism relies on the paracrine effect of stem cells. This procedure of stem cell therapy involves using stem cells isolated from a donor to stimulate the patient’s cells to repair damaged tissues.
Additionally, unlike traditional therapy, stem cells have a wide application. Stem cell therapy is used to manage various degenerative diseases, autoimmune disorders, birth defects, and the research is still ongoing for so many other health conditions where stem cells have shown potential.
Also, there is currently a high demand for aesthetic medicine. Stem cell therapy is a proven alternative to other forms of cosmetology such as plastic surgery. Hence, dermatologists are turning to stem cell therapy to administer anti-aging procedures, skin rejuvenation, hair therapy, micro-needling etc.
The Paracrine effect of stem cells
The paracrine effect of stem cells is one of the most outstanding effects of stem cells. It involves using donor cells to stimulate endogenous repair by harnessing the regenerative power of the human body. It is a mechanism of tissue regeneration that has created new possibilities for managing various conditions using stem cell therapy.
The cells that trigger a paracrine response are; mesenchymal cells, umbilical cord blood, umbilical cord tissue, adipose (fat) tissue and blood cells from a donor’s bone marrow.
The paracrine effect occurs when the donor’s cells send the damaged or defective cells signals to induce self regeneration and repair by secreting some factors and proteins. One of the mechanism by which this paracrine effect is initiated, involves the secretion of cytokines and regulatory proteins by the damaged patient’s cells, these cytokines and proteins act as mediators to stimulate an immune response that attracts the donor cells, this causes the donor cells to release proteins and factors that stimulate the patient’s cells to promote cell proliferation, increase vascularization and blood flow to the areas that needs to heal, while reducing inflammation.
Moreover, research has shown that the paracrine effect of stem cells prevents damaged and diseased cells from dying. They are also therapeutically useful in autoimmune diseases and preventing transplant rejection due to the immune suppression effect they have.
Is stem cell therapy effective?
Doctors are always looking for ways to provide the best possible treatment to their patients, and that is why many clinics are embracing stem cell therapy as a standard, due to its many advantages.
Stem cell therapy is one of the most effective and safest therapy patients can receive, when compared to other existing treatment options. Stem cell therapy is used in promoting patient outcomes in a lot of disease conditions that were previously poorly treated by other alternatives.
Again, as new potentials and ways of applying stem cells are being discovered, doctors are beginning to maximize these benefits in their clinics. Some conditions that are currently treated by stem cells include autoimmune conditions, immunotherapy Car-T cells, chronic obstructive pulmonary disease, neurodegenerative conditions, osteoarthritis, spinal cord injury, aesthetics/anti-aging, sports medicine, autism and multiple sclerosis.
Another reason clinics are adopting stem cell therapy as a standard therapy is because it is easy to administer. A lot of machines such as GCELL {Insert link} which makes the harvesting and processing of stem cells easy and fast, have made the procedures easily adaptable by doctors.
Furthermore, stem cell therapy reduces the treatment and recovery time associated with surgical procedures and other treatment options. This alone is a big factor in why stem cells are becoming a standard therapy in clinics.
Therapeutic uses of stem cells vs traditional medicine
Existing stem cell research has shown how the regenerative effect of stem cells is defining the future of medicine. The major advantage of stem cell therapy over conventional medication-based therapy is its safety. Stem cell therapy is aimed at treating the cause of the disease while traditional medicine targets the symptoms.
Another problem with traditional medical therapy is that it introduces another problem while trying to solve the existing one. As a doctor, you always run the risk of causing harm with each prescription because of various adverse effects that could lead to major organ damage of the kidney, liver etc. On the other hand, patients already know this and they are actively seeking better alternatives, this is why stem cell therapy is fast becoming a standard therapy in clinics.
Moreover, doctors will always be concerned about whether their patients are taking their medications or not. The burden of drug compliance and adherence associated with traditional medical therapy is not always easy to navigate. This is why effective treatment options like stem cell therapy have become a standard therapy in clinics. It only requires the patients having a procedure that repairs and restores damaged cells and tissues in the most natural way.
If you would like to become certified in regenerative medicine using stem cells and other cellular therapy, contact us.
- Published in Corporate News / Blog
GCell: The Newest All-In-One Solution in Regenerative Medicine
Are you a physician that is currently utilizing adipose tissue, but is growing tired of the time-consuming, arduous procedure? Are you having problems finding reagents that allow you to isolate stem cells? If so, GCell might be the solution for you.
What is GCell?
GCell is a revolutionary new machine that holds the potential to become the future of adipose stem cell processing. This is due to a variety of reasons, from the compactness of the unit, to its short processing time– it truly is a valuable implement in any regenerative medicine practitioner’s office. GCell employs a process of mechanical breakdown, which in addition to shortening the duration of the treatment, also serves to keep it within legal minimal-manipulation regulations.
How Does GCell Work?
Through a system of extremely small blades and filters, it is able to homogenize a sample of fat taken from anywhere in the body, making it into a slurry of growth factors, proteins, and the other components that make up the sample. The GCell then filters out the stromal vascular fraction cells, and uses a process called photoactivation to increase their vitality. Once the process is over, the end result is a final product that can be administered to patients within forty minutes from the sample’s harvesting. This is a far cry from the previous, muti-hour long treatments that physicians have grown accustomed to, and this shortened timespan is something that both doctors and their patients will greatly appreciate.

Why GCell?
Additionally, it is a single-session treatment. This means that patients that wish to receive a GCell treatment will only have to visit their clinic once, and will not have to undergo any followup treatments. This machine provides the convenience of its small size and lightweight build with the ability to accelerate the stem cell harvesting process– but that isn’t all. The GCell has been designed to be an entirely enclosed system– this is important, as it means that samples that are run through the GCell will remain in a sterile environment, which preserves the viability of samples and ensures positive outcomes for patients.
The GCell combines a grinder, a filter, and a photoactivation device, and is a turnkey solution that can take a physician from harvesting a fat sample to administering an injectable regenerative medicine therapy in less than an hour. GCell has been designed to be especially useful for clinics that are just beginning to implement regenerative medicine into their practice, but it’s all inclusive approach to stem cell isolation is what sets it a cut above the rest.

GCell’s Single Session Treatment Protocol
Unlike many other cellular therapies on the market, it is a single-session treatment, which means that there is no need for the patient to come back after his original treatment day has ended. This machine’s portability, small stature, and ability to accelerate the stem cell harvesting process makes it ideal for clinics that are just beginning to implement regenerative medicine into their practices, as it takes much of the rigor out of adipose-derived stem cell harvesting.
- Published in Corporate News / Blog
How to boost your immune system to fight cancer?
The human immune system helps to protect the body against illness and infection caused by bacteria, viruses, fungi, and parasites. This process is achieved by a collection of reactions and responses made by the body to damage these infected cells. It is also called immune responses.
This immune system is very crucial in cancer patients to help fight cancer, it dictates this cancer as abnormal and destroys it, but this is not enough to rid of cancer altogether. In most cases, cancer will weaken this immune system because it will spread into the bone marrow that produces blood cells that fights against infections and cause the bone marrow to decrease in its blood cell production.
When this immune system is unable to recognize these cells as abnormal, cellular growth will occur, causing uncontrolled growth and division of cells, that will, in turn, lead to cancer.
Cancer has been a serious and sensitive talk for both patients and doctors. Being diagnosed with cancer is frightening and tormenting, but due to the latest treatment method, recovering from this disease is increasingly possible. Living with cancer often brings an initial psychological crisis, but surprisingly it does not only affect you but your family and others close to you.
Cancers, especially genetic cancer can’t be prevented, so it is essential to be proactive about your health. If you’re diagnosed with cancer, some individual lifestyles that will help improve your cancer care, which includes managing stress. Reducing your stress level can help you to maintain physical and mental stress; you can use relaxation techniques such as meditation and yoga. Getting enough sleep is also crucial for patients living with cancer; this will help improve their health, mood, and coping ability. Also, it is best the limit their exposure to toxins that can increase one’s risk of being exposed to other deadly diseases.
A healthy feeding habit is critically important and can help manage cancer side effects, improve health, and quick recovery. Some tips to help you develop a good and healthy feeding diet include:
- Consuming assorted types of vegetables in all your meals. Vegetables are essential and should not just be a side dish but the centerpiece of your meal.
- Consuming foods rich in fiber like grains, beans, peas, nuts, and seeds.
- Consuming less red meat, like pork, lamb, goat, and bison.
- The presence of probiotic and prebiotic foods helps to support a healthy gut. Probiotic foods include yogurt or other fermented vegetables, and prebiotic foods include raw or cooked onions, dandelion greens, and legumes.
- Avoid processed and canned foods
- Avoid foods high in calories and low in nutrients like fruit-flavored drinks, sodas, candies, and sweets.
- Lastly, cut down on the excessive intake of alcohol.
Some other routines can help improve cancer care like regular exercise. Regular exercise helps to control fatigue, muscle tension, and anxiety in those with cancer, and it is essential, especially during and after cancer treatment, so keep fit and avoid adding unnecessary weight.

CANCER TREATMENT
There are many cancer treatment options for different types of cancers. Cancer treatments depend on the type and how to advance it is. Some patients with cancer will only have one treatment option, while others will end up with a combination of more that one treatments technique depending on the type and stage of cancer.
Curing cancer is one of the significant challenges of the 21st century. However, few advances to tame the immune system are getting closer to a future where cancer can be a curable disease.
Although cancer treatment is dependent on the stage and type, we need a wide range of therapies that work on cellular level like NK cell and stem cell therapies, wide enough to cover the whole spectrum of cancer. Cancer therapies involving the immune system is believed to be a milestone for cancer treatment advances, and the development of multiple immune cells as a therapeutic tool.
Our knowledge of cancer has dramatically improved in recent years. And it seems increasingly evident that there has been a surge of new technologies, and these technologies could make a great impact on the way we treat cancer, taking us closer to finally curing this deadly disease.
NK CELLS
One of these promising cancer treatment advances is the natural killer (NK) cell-based immunotherapy. Natural killer cells have emerged as the newest promising therapeutic approach to cancer. Our understanding of the biological processes that take place in cancer is increasing rapidly, leading to this new type of targeted treatment and therapeutic approach. It is hard to overstate the possible importance of NK cells in the future of cancer. Modern researches have shown that NK cells are a type of treatment that stimulates a persons’ immune system to fight cancer, and this may give room for a greater number of chances to beat cancer for good. NK cells are also known for their ability to target cancer stem cells making these cancer stem cells visible to the immune system.
NK cells was first identified in the 1970s as a unique lymphocyte subset that can recognize and kill abnormal cells without prior sensitization of specific tumor antigen, thus preventing the growth of many cancers. During the late 1980s, something was observed, and this was that NK cells could destroy a lymphoma cell line that had lost MHC class I surface molecules while the original MHC class I+ cells were resistant to lysis, which led to the formation of the “missing self-hypothesis” which states that NK cells can sense the absence of “self” MHC class-I molecule on target cells. In recent years, the hypothesis was confirmed by the inhibitory and activating NK cell receptors.
This discovery indicates that autologous cells are not killed by NK cells, thanks to an appropriate expression of all self-HLA alleles, do not kill an autologous cell. In contrast, a wide spec of cancer types can be killed due to the loss of HLA molecules and to the expression/overexpression of ligands for NK cell activating receptors.
Now, this is how NK therapy works
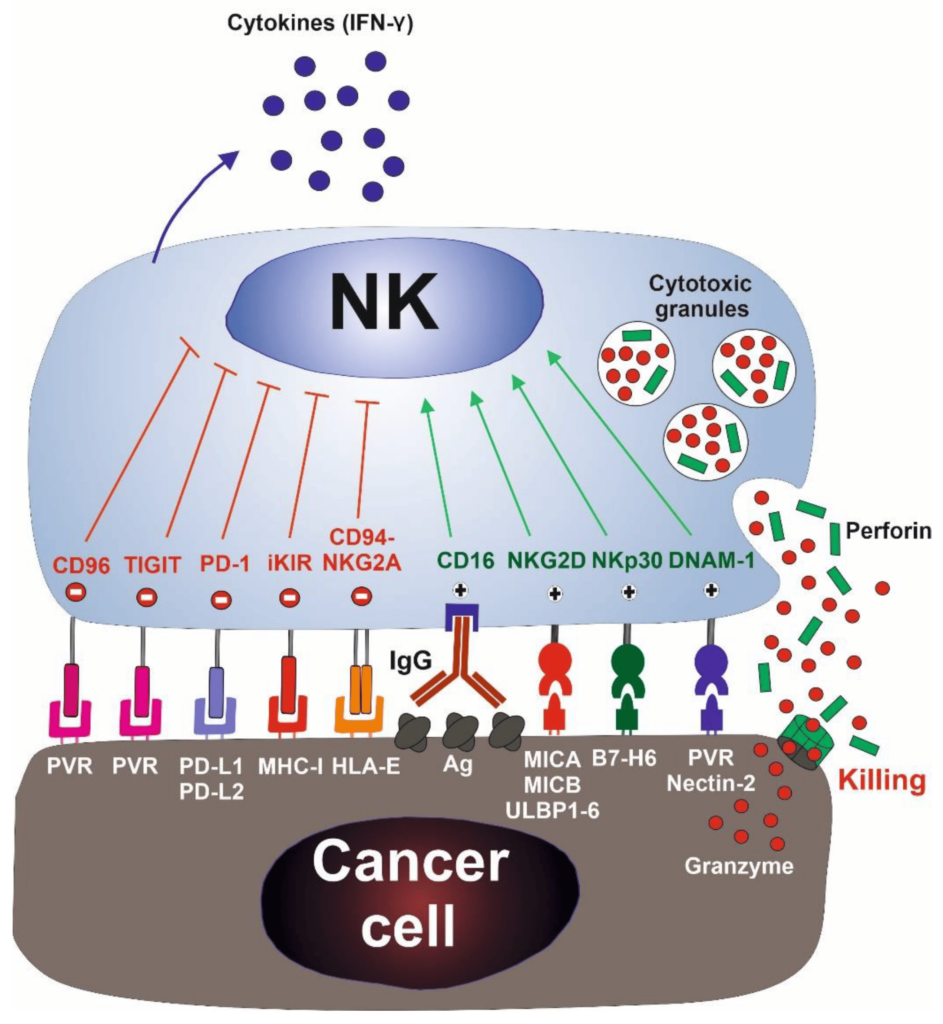
NK cells firsts recognize the tumor cells via stress or danger signals from their sensors.
Then, the Activated NK cells directly decimate the target tumor cells through at least four mechanisms. These mechanisms are cytoplasmic granule release, death receptor-induced apoptosis, effector molecule production, or ADCC.
Furthermore, NK cells act as regulatory cells when reciprocally interact with DCs to improve their antigen uptake and presentation. This action helps in facilitating the generation of antigen-specific CTL responses that is vital in dictating foreign invasion and tumor cells.
Also, by producing cytokines such as IFN-γ, activated NK cells induce CD8+ T cells to become CTLs. Activated NK cells can also help in the differentiation of CD4+ T cells toward a Th1 response and promote CTL differentiation. Cytokines produced by NK cells might even have the unique ability to regulate antitumor cells, making them more proactive.
Accordingly, The cytokine gene transfer approach induces NK cell proliferation, and this increases survival capacity. Further enhancing their activation and also making them more potent in malignant cell multiplication dictation.
The NK cell scientist has assured that by using NK cell lines, modifying genes such as IL-2, IL-12, IL-15, and stem cell factor (SCF). They have been demonstrated the ability of the NK to restore their cytotoxic capacity as well as increase their proliferative rate, survival ability, and in vivo antitumor activity. However, the specificity of NK cells is still limited, and studies are even passing through phases. The approach focuses on retargeting NK cells to tumor cells by gene transfer of chimeric tumor-antigen specific receptors.
NK therapy is promising research; it raises the prospect of “one-end-solution” to many different types of cancers across the Globe. If the studies and experiments work out pretty well, the NK cells will be able to increase the activity of CD4+, CD19, and other important disease-fighting cells of the body.
There is no doubt that this an unimaginable feat, both in advancing our basic knowledge about regenerative medicine and for the possibility of future cancer treatment advances.
- Published in Corporate News / Blog
Clinical trials on NK cells give hope for many people Who are suffering from cancer.
Induced pluripotent stem cells (also known as iPS cells or iPSCs) are a type of pluripotent stem cell that can be generated directly from a somatic cell. Pluripotent stem cells hold promise in the field of regenerative medicine. Because they can propagate indefinitely, as well as give rise to every other cell type in the body (such as neurons, heart, pancreatic, and liver cells), they represent a single source of cells that could be used to replace those lost to damage or disease.
Natural killer cells are the type of cytotoxic lymphocyte critical to the innate immune system. The role NK cells play is analogous to that of cytotoxic T cells in the vertebrate adaptive immune response. NK cells provide rapid responses to virus-infected cells, acting at around three days after infection, and respond to tumor formation.
Typically, immune cells detect the major histocompatibility complex (MHC) presented on infected cell surfaces, triggering cytokine release, causing apoptosis. NK cells are unique, however, as they can recognize stressed cells in the absence of antibodies and MHC, allowing for a much faster immune reaction.
Clinical Trial on NK cells
In a first clinical trial, a natural killer cell immunotherapy derived from induced pluripotent stem cells is being tested for safety in 64 patients with a variety of solid tumors. The first subjects used for the study received the cells in February at the University of California, San Diego (UCSD) Moores Cancer Center and MD Anderson Cancer Center.
This study is targeting late-stage cancer patients with solid tumors, including lymphoma, colorectal cancer, and breast cancer. The FT500 NK cells do not undergo any further alterations and after their derivation from the induced pluripotent stem cells (iPSCs), offering the possibility of a quicker, ready-made treatment.
Human embryonic stem cells induced iPSCs
Human embryonic stem cells (hESCs) and induced pluripotent stem cells (iPSCs) provide an accessible, genetically tractable, and homogenous starting cell population to efficiently study human blood cell development. These cell populations provide platforms to develop new cell-based therapies to treat both malignant and nonmalignant hematological diseases.
The NK cells are immune cells in the same family as T and B cells and are very good at targeting cancer cells for destruction. Some Laboratory experiments have shown they do so by attacking cells that have lost their significant self-recognition signals that tell the immune system not to attack. This is the phenomenon that can happen among cancer cells but not to healthy cells. Experts are not sure how many cancer cells lose that signal. Researchers are hopeful that the clinical trial can help determine which cancer patients could benefit the most from NK cell treatment.
iPS Clone
The ability to induce pluripotent stem cells from committed, human somatic cells provides tremendous potential for regenerative medicine. However, there is a defined neoplastic potential inherent to such reprogramming that must be understood and may offer a model for critical understanding events in the formation of the tumor. Using genome-wide assays, we identify cancer-related epigenetic abnormalities that arise early during reprogramming and persist in induced pluripotent stem cell (iPS) clones. These include hundreds of abnormal gene silencing events, patterns of aberrant responses to epigenetic-modifying drugs resembling those for cancer cells, and presence in iPS and partially reprogrammed cells of cancer-specific gene promoter DNA methylation alterations.
Progress in adoptive T-cell therapy for cancer and infectious diseases is hampered by the lack of readily available antigen-specific, human T lymphocytes. Pluripotent stem cells could provide an estimable source of T lymphocytes, but the therapeutic potential of human pluripotent stem cell-derived lymphoid cells generated to date remains uncertain.
Modification of T cells
Recently, some Approved cell therapies for Cancer also rely on modifying T cells, in those cases to produce cancer cell–binding chimeric antigen receptors (CARs), and have been effective in treating certain cancers such as leukemia.
Application of CAR T-Cell Therapy in Solid tumours
The Car T technology has wowed the field by all but obliterating some patients’ blood cancers, but solid malignancies present new challenges.
Therapies that contains such chimeric antigen receptor (CAR) T cells have been approved for some types of so-called liquid cancers of the blood and bone marrow, large B-cell lymphoma and B-cell acute lymphoblastic leukemia. But the approach has not had as much success for solid tumors.
Serious research into the therapy for brain cancer started almost 20 years ago after cancer biologist WaldemarDebinski, then at Penn State, discovered that the receptor for the immune signaling molecule interleukin 13 (IL-13) was present on glioblastomas, but not on healthy brain tissue. The receptor thus seemed like an excellent target to home in on cancer cells while sparing healthy ones. The CAR spacer domain that spans the immune cells’ membranes and its intracellular co-stimulatory areas, as well as the process used to expand cells outside the body, to boost the T cells’ activity.
CAR T- A Safer Cell Therapy
While managing CAR T-cell therapy toxicity could help keep already-designed treatments on their march to the clinic, many immunotherapy companies are also working to develop a new generation of inherently safer therapies, yet just as efficient. A crucial part of achieving this goal will be improving CAR specificity for target cells. With current treatments, the destruction of normal cells is often an unavoidable side effect when healthy tissue carries the same antigens as tumors; noncancerous B cells, for example, are usually casualties in CD19-targeted therapies.
CAR T delivery is a non-easy factor in the treatment of solid tumors and other unknown forms of tumors. With the non-solid cancers, cells are administered by a blood infusion, and once in circulation, the CAR T can seek out and destroy the rogue cells. For solid tumors, it’s not so simple.
The main drawback of taking cells from a patient and developing them into a cellular immunotherapy product is that the process can take weeks.
Patel tells The Scientist “But for the majority of patients who may not be a candidate or may not have time to wait for such an approach, the idea that there’s off-the-shelf immunotherapy that could potentially as a living drug act against their cancer, I think is a fascinating concept,”
- Published in Corporate News / Blog
Stem cell treatment could offer one-end-solution to Diabetes
Insulin-producing cells grown in the lab could provide a possible cure for the age-long disease (diabetes).
Type 1 diabetes is an auto-immune disease that wipes out insulin-producing pancreatic beta cells from the body and raises blood glucose to dangerously high levels. These high levels of Blood sugar level can be even fatal. Patients are being administered insulin and given other medications to maintain blood sugar level. To those who cannot maintain their blood sugar level, they are given beta-cell transplants but to tolerate beta cell transplants; patients have to take immunosuppressive drugs as well.
A report by a research group at Harvard University tells us that they used insulin-producing cells derived from human embryonic stem cells (ESCs) and induced pluripotent stem cells to lower blood glucose levels in mice. Nowadays, many laboratories are getting rapid progress in human stem cell technology to develop those cells that are functionally equivalent to beta-cells and the other pancreatic cell types. Other groups are developing novel biomaterials to encapsulate such cells and protect them against the immune system without the need for immunosuppressant.
Major pharmaceutical companies and life sciences venture capital firms have invested more than $100 million in each of the three most prominent biotechnological industries to bring such treatments into clinical use:
- Cambridge
- Massachusetts–based companies Semma Therapeutics
- Sigilon Therapeutics, and ViaCyte of San Diego
Researchers of UC San Francisco have transformed human stem cells into mature insulin-producing cells for the first time, a breakthrough in the effort to develop a cure for type-1 (T1) Diabetes. Replacing these cells, which are lost in patients with T1 diabetes, has long been a dream of regenerative medicine, but until now scientists had not been able to find out how to produce cells in a lab dish that work as they do in healthy adults.
What is T1 diabetes?
T1 diabetes is an autoimmune disorder that destroys the insulin-producing beta cells of the pancreas, typically in childhood. Without insulin’s ability to regulate glucose levels in the blood, spikes in blood sugar can cause severe organ damage and eventually death. The condition can be managed by taking regular shots of insulin with meals. However, people with type 1 diabetes still often experience serious health consequences like kidney failure, heart disease and stroke. Patients facing life-threatening complications of their condition may be eligible for a pancreas transplant from a deceased donor, but these are rare, and they are supposed to wait a long time.
Researchers have just made a breakthrough that might one day make these technologies obsolete, by transforming human stem cells into functional insulin-producing cells (also known as beta cells) – at least in mice.
“We can now generate insulin-producing cells that look and act a lot like the pancreatic beta cells you and I have in our bodies,” explains one of the team, Matthias Hebrok from the University of California San Francisco (UCSF).
“This is a critical step towards our goal of creating cells that could be transplanted into patients with diabetes.”
Type-1 diabetes is characterized by a loss of insulin due to the immune system destroying cells in the pancreas – hence, type 1 diabetics need to introduce their insulin manually. Although this is a pretty good system, it’s not perfect.
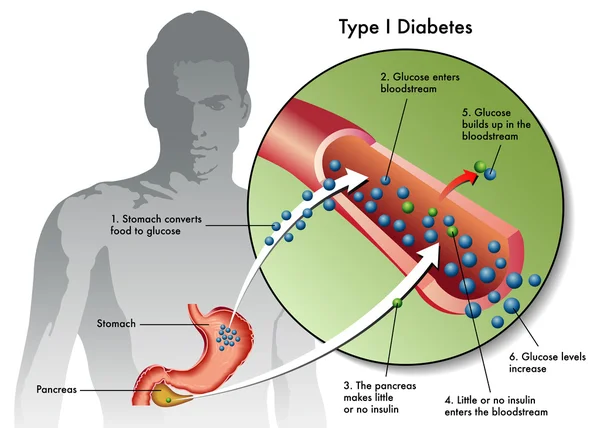
Making insulin-producing cells from stem cells
Diabetes can be cured through an entire pancreas transplant or the transplantation of donor cells that produce insulin, but both of these options are limited because they rely on deceased donors. Scientists had already succeeded in turning stem cells into beta cells, but those cells remained stuck at an early stage in their maturity. That meant they weren’t responsive to blood glucose and weren’t able to secrete insulin in the right way.
Scientists at the University of California San Francisco made a breakthrough in the effort to cure diabetes mellitus type 1.
For the first time, researchers transformed human stem cells into mature insulin-producing cells, which could replace those lost in patients with the autoimmune. There is currently no known way to prevent type-1 (T1) diabetes, which destroys insulin production in the pancreas, limits glucose regulation, and results in high blood sugar levels. The condition can be managed with regular shots of insulin, but people with the disease often experience serious health complications like kidney failure, heart disease, and stroke.
“We can now generate insulin-producing cells that look and act a lot like the pancreatic beta cells you and I have in our bodies,” according to Matthias Hebrok, senior author of a study published last week in the journal Nature Cell Biology.
“This is a critical step toward our goal of creating cells that could be transplanted into patients with diabetes,” Hebrok, director of the UCSF Diabetes Center, said in a statement.
Islets of Langerhans are groupings of cells that contain healthy beta cells, among others. As beta cells develop, they have to separate physically from the pancreas to form these islets.
The team artificially separated the pancreatic stem cells and regrouped them into these islet clusters. When they did this, the cells matured rapidly and become responsive to blood sugar. In fact, the islet clusters developed in ways “never before seen” in a lab. After producing these mature cells, the team transplanted them into mice. Within days, the cells were producing insulin similar to the islets in the mice. While the study has been successful in mice, it still needs to go through more rigorous testing to see if it would work for humans as well. But the research is up-and-coming. “We can now generate insulin-producing cells that look and act a lot like the pancreatic beta cells you and I have in our bodies. This is a critical step towards our goal of creating cells that could be transplanted into patients with diabetes,” He said.
“We’re finally able to move forward on several different fronts that were previously closed to us,” he added. “The possibilities seem endless.”
Basic research keeps elucidating new aspects of beta cells; there seem to be several subtypes, so the gold standard for duplicating the cells is not entirely clear. Today, however, there is “a handful of groups in the world that can generate a cell that looks like a beta cell,” says Hebrok, who currently acts as scientific advisor to Semma and Sigilon, and has previously advised ViaCyte. “Certainly, companies have convinced themselves that what they have achieved is good enough to go into patients.”
The stem cell reprogramming methods that the three companies use to prompt cell differentiation create a mixture of islet cells. Beta cells sit in pancreatic islets of Langerhans alongside other types of endocrine cells. Alpha cells, for example, churn out glucagon, a hormone that stimulates the conversion of glycogen into glucose in the liver and raises blood sugar. Although the companies agree on the positive potential of islet cell mixtures, they take different approaches to developing and differentiating their cells. Semma, which was launched in 2014 to commercialize the Harvard group’s work and counts Novartis among its backers, describes its cells as fully mature, meaning that they are wholly differentiated into beta or other cells before transplantation. “Our cells are virtually indistinguishable from the ones you would isolate from donors,” says Semma chief executive officer BastianoSanna
To get around the donor problem, researchers, including the team at UCSF has been working on nudging stem cells into becoming fully-functional pancreatic beta cells for the last few years. Still, there have been some issues in getting them all the way there.
“The cells we and others were producing were getting stuck at an immature stage where they weren’t able to respond adequately to blood glucose and secrete insulin properly,” Hebrok said.
“It has been a major bottleneck for the field.”
“We’re finally able to move forward on a number of different fronts that were previously closed to us,” Hebrok added. “The possibilities seem endless.”
Regardless of starting cell type, the companies say they are ready to churn out their cells in large numbers. Semma, for example, can make more islet cells in a month than can be isolated from donors in a year in the United States, Sanna says, and the company’s “pristine” cells should perform better than donor islets, which are battered by the aggressive techniques required for their isolation.
As these products, some of which have already entered clinical trials, move toward commercialization, regulatory agencies such as the US Food and Drug Administration (FDA) and the European Medicines Agency have expressed concern about the plasticity of the reprogrammed cells. All three firms subject their cells to rigorous safety testing to ensure that they don’t turn tumorigenic. Before successful trials, companies won’t know the dose of beta cells required for a functional cure, or how long such “cures” will last before needing to be boosted. There’ll be commercial challenges, too: while the companies are investing heavily to develop suitable industrial processes, all acknowledge that no organization has yet manufactured cell therapies in commercial volumes.
Nevertheless, there’s growing confidence throughout the field that these problems will be solved, and soon. “We have the islet cells now,” says Alice Tomei, a biomedical engineer at the University of Miami who directs DRI’s Islet Immuno-engineering Laboratory.
“These stem cell companies are working hard to try to get FDA clearance on the cells.”
Protecting stem cell therapies from the immune system
Whatever the type of cell being used, another major challenge is delivering cells to the patient in a package that guards against immune attack while keeping cells fully functional. Companies are pursuing two main strategies:
- Microencapsulation, where cells are immobilized individually or as small clusters, in tiny blobs of a biocompatible gel.
- Macroencapsulation, in which greater numbers of cells are put into a much larger, implantable device.
ViaCyte, which recently partnered with Johnson & Johnson, launched its first clinical trial in 2014. The trial involved a micro-encapsulation approach that packaged up the company’s partially differentiated, ESC-derived cells into a flat device called the PEC-Encapsulation. About the size of a Band-Aid, the device is implanted under the skin, where the body forms blood vessels around it. “It has a semipermeable membrane that allows the free flow of oxygen, nutrients, and glucose,” says ViaCyte’s chief executive officer, Paul Laikind. “And even proteins like insulin and glucagon can move back and forth across that membrane, but cells cannot.”
The trial showed that the device was safe, well-tolerated, and protected from the adaptive immune system—and that some cells differentiated into working islet cells. But most cells didn’t engraft effectively because a “foreign body response,” a variant of wound healing, clogged the PEC-Encap’s membrane and prevented vascularization. ViaCyte stopped the trial and partnered with W. L. Gore & Associates, the maker of Gore-Tex, to engineer a new membrane. “With this new membrane,” says Laikind, “we’re not eliminating that foreign body response, but we’re overcoming it in such a way that allows vascularization to take place.” The company expects to resume the trial in the second half of this year, provided it receives the green light from the FDA.
Semma is also developing macro¬-encapsulation methods, including a very thin device that in prototype form is about the size of a silver dollar coin. The device is “deceptively simple, but it allows us to put [in] a fully curative dose of islets,” Sanna says.
Semma is also investigating microencapsulation alternatives. At the same time, the company is advancing toward clinical trials using established transplantation techniques to administer donated cadaver cells to high-risk patients who find it particularly difficult to control their blood glucose levels. These cells are infused via the portal vein into the liver, and patients take immunosuppressive drugs to prevent rejection.
Sigilon is working on its microencapsulation technology. Launched in 2016 on the back of work by the labs of Robert Langer and Daniel Anderson at MIT, the company has created 1.5-millimeter gel-based spheres that can hold between 5,000 and 30,000 cells (Nat Med, 22:306–11, 2016). Each sphere is like a balloon, with the outside chemically modified to provide immune-protection, says Sigilon chief executive officer Rogerio Vivaldi. “The inside of the balloon is full of a gel that creates almost a kind of a matrix net where the cells reside.”
In 2018, shortly after partnering with Eli Lilly, Sigilon and collaborators published research showing that islet cells that were encapsulated in gel spheres and transplanted into macaques remained functional for four months. The company has not disclosed a time frame for a type 1 diabetes trial “but we’re moving pretty quickly,” says chief scientific officer David Moller.
Conclusion
To conclude, all three firms hope to extend their work to treat some of the 400 million people worldwide with type 2 diabetes, many of them eventually benefit from insulin injections. The recent endorsements from big Pharmaceutical underline the real progress in beta-cell transplants, says Aaron Kowalski, a molecular geneticist and chief executive officer at JDRF, a foundation based in New York that has funded research at ViaCyte and academic labs whose work has been tapped by Semma and Sigilon. “These companies all realize that if they don’t do it, somebody else will. It’s hard to predict exactly when, but somebody is going to make this work.”
- Published in Corporate News / Blog
Bats Carry Corona Virus. So Why Don’t They Get Sick?
A lot of viruses that has taken a toll on life, the ebola virus in Africa, The Nipah virus of Nipah and the most recent one corona virus that left china running helter skelter all seemed to have originated from bats. During the course of the virus epidemic in Wuhan where it was first detected, some Chinese researchers in Wuhan examined some patients affected in that area and then took samples of the virus. They did findings on the genetic sequence of the virus with other viruses that were known. The corona virus surprisingly had a 96% match with the horseshoe bats that are dominant in the southwest of china. The research findings were then published in a study on February, 2020.
A virologist Vineet Menachery from the university of Texas Medical Branch at Galveston though not affiliated to the study said “They’re too close in terms of their pure genetics to say they’re not related, or that they didn’t have a common ancestor.” Menachery was a reputable virologist and had done other research works. He contributed to the theory that the spread of the corona virus must have been from these bats to humans. And possibly must have had another animal that served as an intermediary for the spread.
This same thing had happened with other forms of corona viruses as noted in the case of SARS (Severe Acute Respiratory Syndrome) an outbreak that took place in 2002-2003 where civets, a mongoose family member were infected with the bat corona virus and spread as humans bought them for food.
Another case was the MERS (Middle East Respiratory Syndrome) outbreak. This one happened in 2012 and was as a result of infected camels from the virus. People who ate undercooked meat of camels and as well drank the raw milk of camels were all affected.
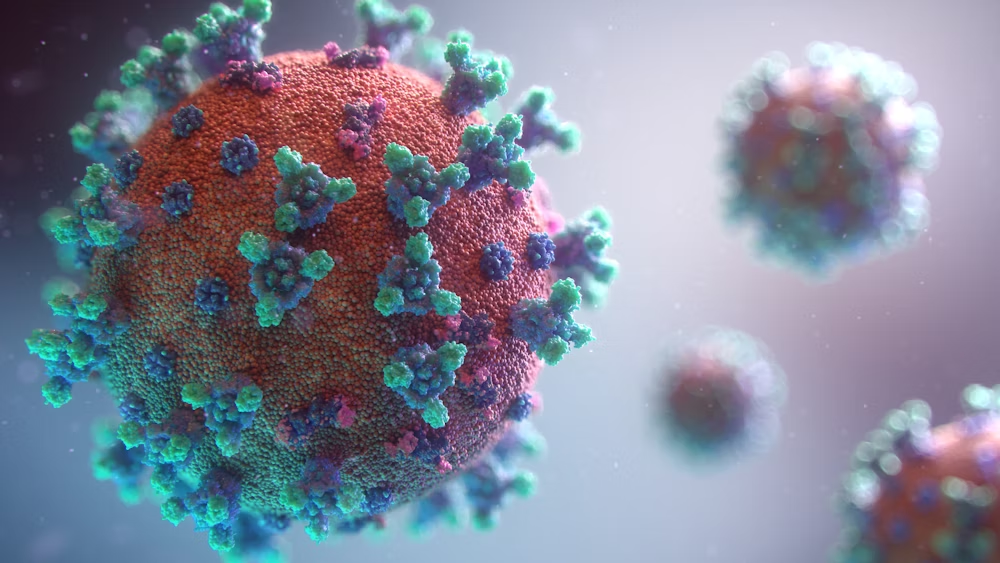
So why is it that there are so many diseases that are spread from bats?
Its no doubt, bats have a lot of viruses that they carry with them. And these viruses in their variety are spread and manifests its tolls on people. Scientist are not sure why this is the case as confirmed by Kevin Olival, a research vice president as EcoHealth Alliance, a non-profit organization based in the U.S. He went further to say that it may have something to do with the family of the viruses carried by the bats. So you know, there are over 130 different families of viruses that bats do carry around. And then, most bats and humans do come in contact through several means. The millions of populations of bats are ubiquitous to all the continents apart from in antartica. Rebekah of Colorado State university who researched infectious pathogens said “There’s a lot of viruses we’re finding in bats because there’s a lot of bats out there.”
They move about in multitudes and live in colonies of large populations. Some these members live in caves and share caves and trees where there can be a contact between humans and bats. Hence, these viruses can spread from these bats to humans. Despite their sizes, bats have relatively long lifespans and can live over 30 years.”So there’s a long time for them to be persistently infected with the virus and shed it into the environment,” Kading says. The mode of mechanisms for these viruses are through urine, saliva and feces of bats. The outbreak of Nivah that happened in Bangladesh was linked to the sap of a date palm gotten from some trees that some bats licked and had infested with their urine.
Reading through all these, it is not absurd to wonder why the bats themselves do not get affected by the viruses they carry. The answer to that question is based on the fact that the bat is the only flying mammal in the world. Their body metabolism and process quite differ from that of normal mammals too. When bats fly, their heart rates rise to about a thousand beats per minute with a temperature rise of about 100 degrees Fahrenheit. Linfa Wang a student of bat viruses at Duke-NUS Medical School in Singapore says that when these signs manifest in other mammals, they are signals that can trigger death. But this is not the same case for other bats. This is a lifestyle for them, every day. Their system is also capable of producing molecules that other organisms do not have. The molecules carry out repair functions and prevent cell damage. This makes their system a bit irresistible to infections and also make them recalcitrant to viruses and resilient to diseases such as diabetes, cancer and other health conditions.
This is a prove that the manifestation of viruses in mammals is not always as a result of the virus itself, but as a result of the body’s reaction to the presence of such a virus that makes us ill by triggering other chain reactions, as Wang explains.
Olival at EcoHealth explains that these bats have coevolved with these viruses and it is not totally their fault that we humans are infected and affected by these viruses. The actual problem is when the viruses move from their species to other species of mammals which is also fostered by human activity.
Naturally, it would be hard for most animals and mammals to cross paths. But Olivial says that the presence of some activities and availability of exchange platforms made available by humans can allow such interaction to occur. She gave an example using wildlife markets like the one in Wuhan, where a bat could be mixed up with a civet. Who later on come in contact with humans – eg. Butchers who do not observe proper hygiene and protection from animal blood.
“The way that we’re coming into contact with these animals, hunting, selling, and trading them is to a scale that really we haven’t seen before,” he says. Investigative teams did some in-depth search and they discovered some traces of this virus in 22 stalls and in a garbage truck that was found at Huanan Seafood Market right there in Wuhan, a place known for booming trade for live animals. This discovery led to shutting down the market as it was tied to majority of the cases.
The intermediary animals to this viruses are still a mystery, but it is clear that some of these animals are prone to interact more with humans. This is why when they are infected, the likelihood for human infection is widened. These other infected animals can sneeze, urinate, be cooked as food or even owned as pets. Bats are not just vectors for viruses, they play an important role in balancing the eco-system. They feed on insects and fruits and are active agents of pollination. In fact, Wang believes that since these bats have successfully coevolved with these viruses, there is every possibility that they can be the agents that can lead to the cure and provision of therapies for these viruses.
- Published in Corporate News / Blog







![Secondary-Diabetes[1]](https://www.stemcellsgroup.com/wp-content/uploads/2020/02/Secondary-Diabetes1-460x260_c.png)

