German Stem Cell Scientists Develop 3-D “Mini-retinas” –New Hope for Restoring Sight in Patients with Retinal Degeneration Caused by Diabetes and Inherited Disorders.
Breakthrough in Retinal Regeneration Using 3D Organoids
Protocol for 3D Mini-retinas

German researchers have achieved a significant breakthrough in stem cell technology focused on restoring sight through the development of 3D retina organoids. Published in Stem Cell Reports in March, this study leverages the self-organizing properties of stem cells to create complex, multi-cellular tissue structures.
The innovative protocol involves dividing organoids grown from stem cells into three half-moon shaped pieces during early eye development. This technique facilitates the growth of fully functional retinal cells within each segment, including cone photoreceptors crucial for high acuity and color vision. These advancements are particularly promising for patients suffering from retinal degenerative disorders caused by diabetes and inherited conditions.
Advantages of 3D Retinal Organoids
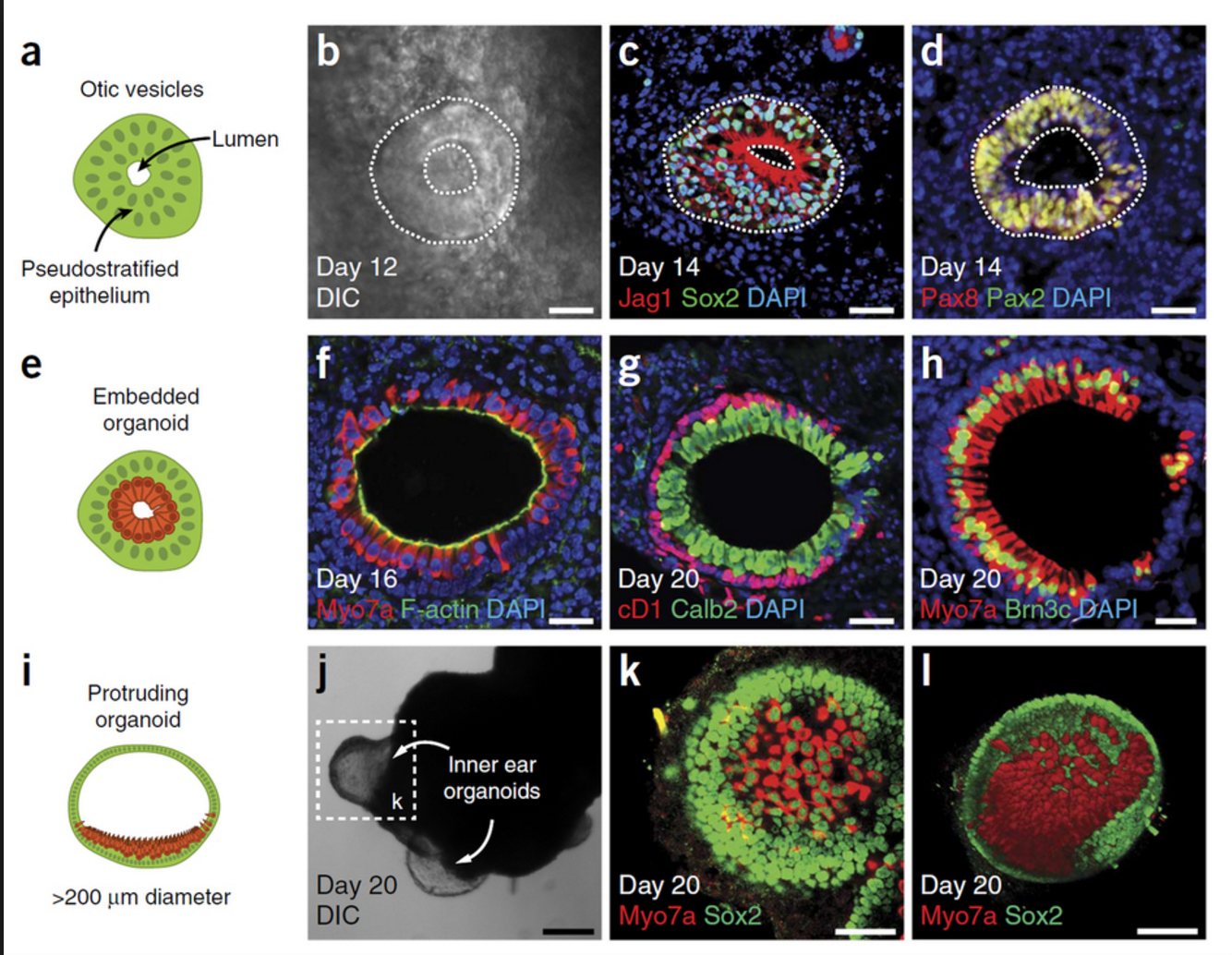
The development process not only enhances the production yield of retinal organoids by up to four times compared to previous methods but also allows for the formation of more realistic tissue structures resembling natural retinal tissue during development.
Applications in Retinal Disease Research
According to senior author Mike Karl from the German Center for Neurodegenerative Diseases (DZNE) and the Center for Regenerative Therapies (CRTD) at Technische Universität Dresden, the versatility of 3D mini-retinas extends beyond replication of retinal tissue. It offers diverse opportunities for studying retinal diseases and potential therapeutic interventions.
Future Directions in Organoid Research
Karl’s team aims to enhance the complexity of mini-retinas by incorporating blood vessels and studying the regeneration capabilities and neural cell functions specific to the human retina. This approach not only furthers understanding of retinal diseases but also holds promise for developing personalized treatments.
Insights and Comparative Studies
Comparative studies between human pluripotent stem cell-derived retina organoids and in vivo mouse retina underscore the potential of this novel organoid protocol to model retinal diseases effectively.
- Published in Corporate News / Blog