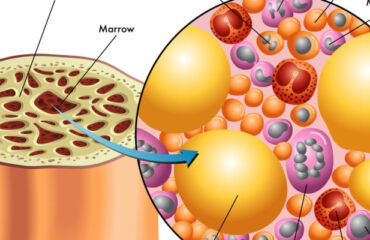
Bone loss and weakening are natural effects of aging, beginning as early as age 30. Factors like smoking, inadequate calcium intake, certain medications, and hormonal changes accelerate bone resorption, leading to decreased density, porous bones, and increased fracture risk.
Stem Cell Innovations in Bone Reconstruction
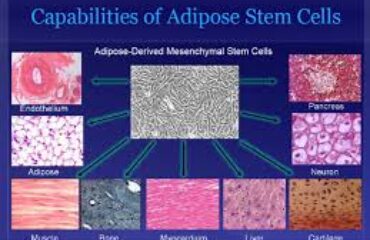
Researchers at the Gladstone Institutes have pioneered a method using proteins derived from stem cells to stimulate bone reconstruction. Unlike traditional methods that rely on bone grafts from cadavers, this approach extracts bone-forming proteins directly from stem cells.
Advantages of Stem Cell Proteins
In experiments on mice, proteins extracted from stem cells were injected into muscle tissue, promoting significant bone growth without the risks associated with traditional bone grafts. This method shows promise for safer, more effective bone repair in humans, with lower rejection and tumor formation risks [1].
Scientific Validation and Clinical Applications
A study published in Scientific Reports affirmed that stem cell-derived proteins offer a reliable source for tissue regeneration. This builds on earlier research, such as Dr. Ranieri Cancedda’s pioneering work using bone marrow cells to repair bone defects [2].
Cutting-Edge Research and Future Directions
Researchers at the National Institutes of Health successfully grew new bone from stem cells derived from skin cells, published in Cell Reports. By reprogramming skin cells into induced pluripotent stem cells (iPSCs) and differentiating them into bone cell precursors, they achieved bone growth in primates without tumor formation. This method harnesses the immune compatibility and versatility of iPSCs, heralding new possibilities for personalized bone regeneration [3].
Conclusion
While the use of stem cells in bone regeneration is advancing, ongoing research aims to refine techniques for optimal integration and long-term effectiveness in human patients.