Platelet-Rich Plasma Stays Quietly Popular Despite Neglect
Fact: PRP Treatments Are Highly In-Demand
According to research, PRP treatments are one of the most in-demand treatments available in healthcare. This is impressive considering the following challenges PRP faces:
- Lack of Support from the Medical Industry: PRP is not backed by big pharma, meaning no extensive research or marketing is funded.
- Absence of Lobbying by Medical Associations: There are no medical associations working to increase awareness of PRP.
- No Insurance Reimbursements: Insurance companies do not reimburse PRP treatments, making it difficult to get patients to pay for a treatment that is relatively “unproven.”
- Rising Costs: In 2006, a PRP treatment cost $450. Today, it costs $800, with the cheapest being $650.
Despite these obstacles, the demand for PRP treatments remains robust.
The Future of PRP
We believe the best of PRP is yet to come. A breakthrough study could propel PRP into mainstream hospitals and clinics. The most significant growth in PRP is currently happening in Asia, rooted in fundamental healing theory.
The Healing Power of PRP
The growth of PRP can be attributed to its fundamental healing properties:
- Increased Platelets: More platelets mean more growth factors and cytokines, leading to enhanced healing.
- Natural Healing Mechanism: Our body’s natural healing mechanism operates with 150,000/ul-350,000/ul platelets in blood. Using PRP amplifies this number by 3X to 5X, translating to better healing.
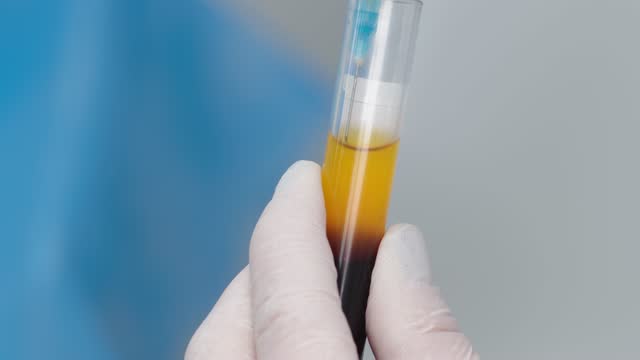
Platelet-Rich Plasma Trends
PRP can be used to promote the healing of injured tendons, ligaments, muscles, and joints, and is applied to various musculoskeletal problems. Regular studies test its effectiveness. One landmark study involved double-blind randomized controlled trials to see the effect of PRP on patients with chronic low back pain caused by torn discs. The study found that 60% of the patients felt significant improvements, with some even being cured.
Platelet-Rich Plasma Variants
There are several types of PRP variants:
- Plasma Rich in Growth Factors (PRGF)
- Plasma Rich in Platelets and Growth Factors (PRPGF)
- Platelet-Rich Plasma (PRP)
- Platelet Poor Plasma (PPP)
- Plasma Rich in Platelets and Rich in Leukocytes (LR-PRP)
- Plasma Rich in Platelets and Poor in Leukocytes (LP-PRP)
- Platelet-Rich Fibrin Matrix (PRFM)
All of them involve plasmapheresis—the two-stage centrifugation process to separate platelets from blood. The industry has yet to standardize which variant to use, but we believe the confusion will clear up in 3-5 years.
Bio-Factors at Play in PRP
Regardless of the PRP variant used, the following bio-factors are at play:
- Growth Factors: TGF-B, PDGF, IGF-I,II, FGF, EGF, VEGF, ECGF
- Adhesive Proteins: Fibrinogen, Fibronectin, Vitronectin, Thrombospondin-1
- Clotting & Anti-Clotting Factors: Proteins, Antithrombin, Plasminogen, Proteases, Antiproteases
How Platelet-Rich Plasma Actually Works
PRP is commonly used for wound healing and pain management because platelets aid coagulation, act as a biological glue, and support stem or primary cell migration. They also help restore hyaluronic acid, accelerate collagen synthesis, and increase cartilage matrix.
Platelets delivered in a clot can immediately act as a scaffold to enable the healing process. 95% of bio-active proteins are released within 1 hour of injecting PRP, and platelets continue to release growth factors for 7-10 days. Thus, it’s recommended to re-inject PRP every 7 days.
Why Patients Choose PRP Despite the Cost
Patients are willing to pay out of pocket for PRP treatments despite insurance companies not covering it because:
- Effectiveness: The treatment works.
- Natural and Side-Effect-Free: There is nothing else as natural and side-effect-free as PRP.
PRP for Osteoarthritis
Consider osteoarthritis, which affects 27 million Americans. When doctors started doing PRP treatments for their osteoarthritis patients, a large majority experienced no further cartilage loss. This suggests PRP should be the default first-line treatment for osteoarthritis across the country.
PRP for Hair Loss and Cosmetic Applications
PRP also has significant potential in treating hair loss and cosmetic facial applications. Studies have shown reduced hair loss and increased hair density, with patients expressing high satisfaction levels.
The Growing PRP Market
The PRP market is expected to hit $126 million in 2016, a 180% increase over the 2009 figure of $45 million. For osteoarthritis alone, if all 27 million Americans received 1 PRP shot a year at a conservative $400 per treatment, it would be a $10 billion market.
PRP for Tennis Elbow
PRP is also known to work well for Tennis Elbow, which affects 1% to 3% of the overall population and up to 50% of tennis players.
Insurance Coverage for PRP
Getting PRP covered by insurance could significantly expand the market and help heal millions of patients more naturally and effectively. It could also save insurance companies money by reducing the need for more expensive interventions like surgery.
Challenges and the Future of PRP
The vast scope of PRP treatment calls for urgent structure and guidelines. There are some 20+ conditions where researchers have found it helpful. Proving its efficiency in all these areas is a daunting task, but we will get there with enough funding and standardized procedures.
Conclusion
Despite being classified as “unproven,” PRP has vast potential. With the right number of platelets, platelet activation, and cytokine release, PRP can consistently deliver positive outcomes. Although there is still uncertainty over the number of injections, timing, and delivery method, widespread adoption will eventually lead to a more structured approach.
Let’s hope the first glimpses of this structure will arrive soon. In 2015, the world saw approximately 1 million knee arthroplasties for osteoarthritis, costing $25 billion. How many of these patients could have benefited from PRP early on?
- Published in Corporate News / Blog
Global Stem Cells Group and Adimarket to Represent Magellan in Latin America and Middle East
Global Stem Cells Group and its subsidiary Adimarket named representatives for Magellan Autologous Platelet Separator in Latin America and Middle East.
MIAMI, Nov. 29, 2017— Global Stem Cells Group (GSCG), a world leader in stem cell and regenerative medicine, and its subsidiary Adimarket have been named to represent the Magellan Autologous Platelet Separator in Latin America and Middle East.
Developed by Arteriorcyte Medical Systems, a leading medical device company headquartered in Hopkinton, Mass., the Magellan Autologous Platelet Separator is a high-tech, automated dual spin processing system designed for use in clinical laboratories or intraoperatively at the point-of-care for safe and rapid preparation of high-quality, platelet-rich plasma (PRP) as well as platelet poor plasma (PPP).
Global Stem Cells Group CEO Benito Novas says the Magellan system is a perfect fit for GSCG and Adimarket’s ever-growing list of high-tech regenerative medicine products and equipment, made available to physicians and qualified practitioners through the Adimarket online store.
“We share Arteriocyte’s commitment to research and development of blood component technology to advance treatments that benefit patients in the field of regenerative medicine,” Novas says. “The Magellan system furthers GSCG’s drive to invest in platelet separation technologies that focus on the development of new surgical applications for PRP and elevates these technologies to the next level.”
The fully-automated Magellan system is specifically designed to fractionate blood at bedside without a need for manual manipulation. At the end of its cycle, the Magellan PRP is delivered into a collection syringe, ready for immediate application.
As an industry leader, Adimarket added the Magellan Autologous Platelet Separator System to its online regenerative medicine store to allow physicians to meet the specific needs of each patient with fully customizable product volumes and platelet concentrations. The system can be programmed to deliver a volume of 3 – 10 mL from each processing cycle, allowing practitioners to customize the concentration per mL within the PRP. The Magellan system is approved for three processing cycles per disposable separation chamber, allowing for a maximum of 30 mL of product.
For more information, visit the Adimarket regenerative medicine online store website, email info@stemcellsgroup.com, or call 305-560-5337.
About Global Stem Cells Group:

Global Stem Cells Group (GSCG) Global Stem Cells Group (GSCG) is a worldwide network that combines seven major medical corporations, each focused on furthering scientific and technological advancements to lead cutting-edge stem cell development, treatments, and training. The united efforts of GSCG’s affiliate companies provide medical practitioners with a one-stop hub for stem cell solutions that adhere to the highest medical standards.
Global stem cell’s mission is to be the largest recognized stem cell and regenerative medicine network in the world.
About Adimarket:
 Adimarket, Inc., a division of the Global Stem Cells Group, is a one-stop, cost-competitive online marketplace for quality regenerative medicine equipment and supplies for physicians and health care professionals.
Adimarket, Inc., a division of the Global Stem Cells Group, is a one-stop, cost-competitive online marketplace for quality regenerative medicine equipment and supplies for physicians and health care professionals.Adimarket was founded to provide practitioners the tools they need to practice regenerative medicine in a medical office setting. Motivated by a firm belief in the impact stem cell medicine can have when dispensed in a doctor’s office, Adimarket provides physicians with the tools they need to provide patients with cutting-edge treatments.
About Arteriorcyte Medical Systems:
 Arteriocyte Medical Systems, Inc. is a leading medical device company committed to developing and marketing novel medical products to help patients heal faster. Established in 2007 by Arteriocyte, Inc. and DW Healthcare Partners, Arteriocyte Medical Systems is devoted to providing innovative solutions to patients and medical professionals to address serious unmet medical needs particularly in cardiac, orthopedic and vascular surgeries.
Arteriocyte Medical Systems, Inc. is a leading medical device company committed to developing and marketing novel medical products to help patients heal faster. Established in 2007 by Arteriocyte, Inc. and DW Healthcare Partners, Arteriocyte Medical Systems is devoted to providing innovative solutions to patients and medical professionals to address serious unmet medical needs particularly in cardiac, orthopedic and vascular surgeries.###
Magellan Autologous platelet separator
- Published in Press Releases